When headlines this summer warned that extreme high rainfall had forced cities and counties to release untreated or partially treated wastewater into Tampa Bay and its tributaries, bay managers were surprisingly silent. From a public perspective, raw sewage is a horrifying concept, conjuring up images of people afflicted with terrible diseases and seagrasses dying by the acres.
People more intimately involved in water quality know that fecal contamination is the norm. Although the millions of gallons of sewage lost last summer are certainly newsworthy, even appropriately treated wastewater may contain bacteria and viruses, as well as nutrients and smaller quantities of pharmaceuticals and micro-plastics. Many tributaries in counties bordering the bay already are considered “impaired” with higher-than-allowed levels of Escherichia coli, the mostly benign bacteria from sewage as well as pets and agriculture that is used to track fecal contamination.
Bay managers aren’t happy about the overflows – and strongly support funding that would fix the problem – but they’re not overly concerned with the events of this summer either.
Roger Johansson, for instance, has been working on Tampa Bay since 1978 and recently retired as director of the City of Tampa’s Bay Study Group, the research organization created to track the changes in the Bay when the city’s first advanced wastewater treatment went online. “The millions of gallons of untreated sewage this summer was just a couple of days’ worth of what was dumped in the Bay for decades,” he says.
“It’s not good but it’s not life-threatening,” he adds. “It’s a temporary problem – we’ve seen chlorophyll a (a phytoplankton used as an indicator of water quality and clarity) go up in Old Tampa Bay and Middle Tampa Bay, but it’s not that bad.”
And while it’s difficult to track an impact to human health, Valerie Harwood, chair of the Department of Integrative Biology at the University of South Florida, isn’t particularly worried either.
“We measured very high levels of fecal contamination in my neighborhood in Temple Terrace and along Bayshore Boulevard in August due to the flooding that allowed contact with the sewage collection system, but didn’t see any illness,” she said.
That’s partially because the most likely illness – gastroterteris caused by Salmonella enterica or other microbes – isn’t necessarily reported. “Most people will experience a few days of nausea, vomiting and diarrhea. Even if it gets bad enough that they go to the doctor, they’ll probably just get Immodium and there’s no good way for a doctor to report it.”
What concerns Harwood more is the viruses that could cause more significant illnesses – but without a better reporting system in place, the data isn’t clear.
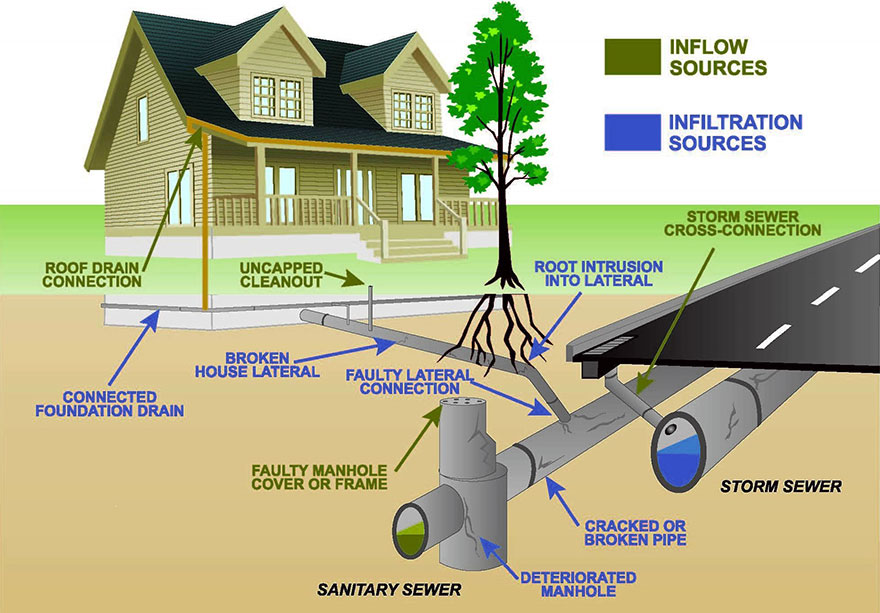
Not all fecal contamination created equal
The problem is that most communities track fecal contamination using E. coli, which can come from any number of warm-blooded sources including humans, dogs, cattle and even birds. The U.S. Environmental Protection Agency sets limits on the levels of E. coli in water, but the sources are determined by land uses, not actually identifying where the contaminant came from.
Fecal matter from humans is far more likely to be dangerous than contamination caused by other animals, because many bacteria, viruses and parasites are host-specific. Although there is some overlap, dogs don’t typically catch colds from human beings and humans don’t get distemper or parvo from dogs. Cattle, however, are greater concern because they are a relatively high-risk source of contamination due to E. coli O157:H7 and Cryptosporidium, a parasite that can cause diarrhea.
With money from an Environmental Protection Commission of Hillsborough County’s pollution recovery grant fund, Harwood and her team are tracking sources of fecal contamination in local waters. “We know they’re impaired but we don’t necessarily know what’s causing it – and we can’t do anything about it until we know where it’s coming from.”
Using E. coli as an indicator can create false positives – or not identify pathogenic viruses. “In some cases, particularly in warm water, E. coli can grow after it enters the water, creating high levels of what appears to be fecal contamination but is not indicative of an ongoing source or a potential danger.”
On the other hand, pathogens that could cause harm to humans aren’t being measured because the technology is so expensive. “Major outbreaks of disease caused by waterborne pathogens are rare in the U.S. because we have good systems in place for treating wastewater and drinking water, but over 700,000 people have become ill and almost 9,000 have died from cholera since the 2010 earthquake in Haiti,” she notes.
Harwood uses a technology called microbial source tracking – or MST – to identify DNA on the bacteria and viruses. DNA is tested – at a cost beginning about a couple of hundred dollars per sample – to clearly identify where the bacteria or virus came from.
In Hillsborough County, for instance, water could be carrying contaminants from pets, cattle, wildlife or people. “What ends up happening is that farmers blame septic systems and residents blame the farmers. If we could definitely identify the source, it would be a giant step toward cleaning it up.”
In other cases, fixing the problem will be more difficult. High levels of contaminants in a wilderness preserve are probably caused by birds and other wildlife so there’s little to be done. “Nobody would want to kill the birds to control the contamination so we can’t do anything about that except warn people not to drink the water,” she said.
El Niño safety steps
With one of the strongest El Nino weather patterns ever recorded threatening to double the winter’s average rainfall, Tampa Bay residents could once again face flooding and potential releases of untreated wastewater.
An international phenomenon, El Niño events occur when tropical Pacific Ocean trade winds drop and ocean temperatures become unusually warm. They bring colder, wetter winters to Florida along with an increased potential for extremely strong tornadoes.
While average rainfall for December to March in the Tampa Bay region is about 10 inches, more than 36 inches fell during the 1997-1998 El Niño. That compares to just 16.47 inches in August – the third wettest August since records were kept beginning in 1890.
Although we can’t change weather patterns, residents can take steps to prevent wastewater from being released into the Bay – and protect their own health:
- Avoid contact with floodwaters and thoroughly wash exposed areas with soapy water. Do not allow children to play in floodwaters.
- Minimize your use of water during heavy rainfall events. Do laundry only as necessary, run dishwashers only when they are full and take shorter showers. All these uses create wastewater that may not be dangerous but must be treated before it is released.
- Check to make sure your irrigation system is turned off. It shouldn’t be running in heavy rains but any additional water can create issues.
- Before rains start falling, repair leaks, including leaky faucets and running toilets. Also consider installing efficient showerheads, dishwashers, and other appliances – you’ll save money in the long run even if weather forecasts don’t actually happen.
- Now is also a good time to think about installing a rain garden to capture stormwater before it has a chance to infiltrate wastewater pipes. Check out http://buildgreen.ufl.edu/Fact_sheet_Bioretention_Basins_Rain_Gardens.pdf for ideas.